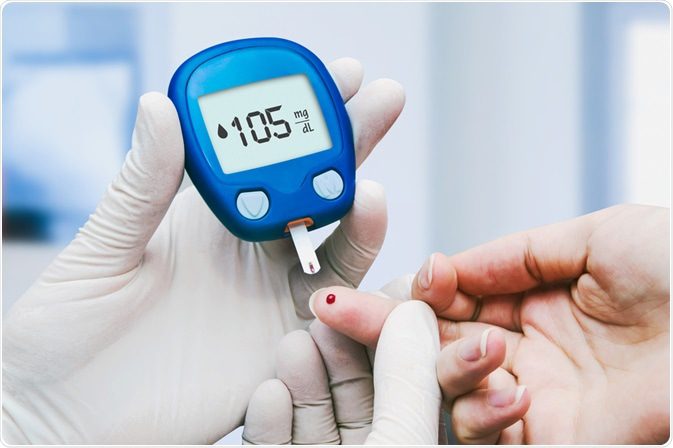
It might be tough to keep your blood sugar levels within the doctor’s recommended range. That’s because a variety of factors may cause your blood sugar levels to fluctuate, sometimes unexpectedly. Some things that might alter your blood sugar levels are listed below. In this article, we will talk all about Diabetes. Know Diabetes tips, Diabetes symptoms, and Diabetic diet.
People with type 2 should know that if you are overweight or obese then you are in a danger zone. As it causes high blood pressure and high cholesterol, which will lead to cardiovascular disease.
So in this article, we are helping you start healthy living with diabetes.
Diabetes symptoms
Some common diabetes symptoms are:
- Urinate (pee) a lot, often at night.
- Are very thirsty.
- Lose weight without trying.
- Are very hungry.
- Have a blurry vision.
- Have numb or tingling hands or feet.
- Feel very tired.
- Have very dry skin.
Diabetic diet: What to eat
Healthy nutrition is an important part of having a healthy lifestyle, whether you have diabetes or not. However, if you have diabetes, you must understand how different meals impact your blood sugar levels. It’s not only what you consume, but also how much you eat and how you combine different kinds of food.
Diabetes tips for you:
What you should do if you have diabetes?
One of the most important diabetes tips is to Learn about portion proportions and carbohydrate counting. Learning how to calculate carbs is an important part of many type 2 diabetes control strategies. It’s critical for individuals who use mealtime insulin to know how many carbs are in their diet so they can obtain the right insulin dosage.
Learn how much of each food group you should consume. Write down amounts for things you consume often to make meal planning easier. Use measuring cups or a scale to ensure proper portion size and a precise carbohydrate count.
Another tip from our diabetes tips box is to Make sure that each meal is well-balanced. Plan for a decent variety of carbs, fruits and vegetables, proteins, and fats in each meal. Pay attention to the carbohydrate you choose. Check out some of these healthy recipes.

Some carbs are healthier for you than others, such as fruits, vegetables, and whole grains. These meals are low in carbs and high in fiber, which helps to stabilize blood sugar levels. Consult your doctor, nurse, or nutritionist for advice on the healthiest foods to eat and the right mix of food kinds.
Make sure your meals and meds are in sync. Low blood sugar might be harmful if you eat too little food in relation to your treatment for diabetes, particularly insulin (hypoglycemia). A high blood sugar level may be caused by eating too much food (hyperglycemia). Discuss how to effectively coordinate meal and medication schedules with your diabetic health care team.
Sugar-sweetened drinks should be avoided. Sugar-sweetened drinks are often heavy in calories and low in nutrients. If you have diabetes treatment food, you should avoid these beverages since they cause blood sugar to increase fast.
Exercise
Physical exercise is an essential component of your diabetes test control strategy. Your muscles utilize sugar (glucose) for energy while you work out. Regular physical exercise also aids in the effective utilization of insulin by the body.
These elements work together to help you reduce your blood sugar. The longer the effect lasts, the more rigorous the exercise. However, even simple tasks like cleaning, gardening, or standing for long periods of time might help you manage your blood sugar. Check out some of the most effective exercises you can do at home.
What you should do?
Consult your doctor about a workout routine. Consult your doctor to determine the best kind of exercise for you. Most individuals should engage in at least 150 minutes of moderate aerobic exercise each week. On most days of the week, aim for 30 minutes of moderate aerobic exercise.
If you haven’t exercised in a long time, your doctor may want to check your overall health before recommending anything. He or she can suggest the ideal aerobic and muscle-strengthening exercise for you.
Maintain a regular workout routine. Consult your doctor about the optimal time of day to exercise so that your workouts are in sync with your eating and medication regimens.
You should be aware of your numbers. Before you start exercising, talk to your doctor about what blood sugar levels are acceptable for you.
Keep an eye on your blood sugar level. Check your blood sugar before, during, and after exercise, particularly if you’re on insulin or other blood-sugar-lowering drugs. Exercise may drop blood sugar levels for up to a day after you’ve done it, particularly if it’s a new activity for you or if you’re doing it at a higher intensity. Low blood sugar might make you feel shaky, weak, tired, hungry, or bewildered.
If you take insulin and your blood sugar level is less than 90 mg/dL (5.0 mmol/L), have a little snack before you begin exercising to avoid a low blood sugar level.
Keep yourself hydrated. Dehydration may alter blood sugar levels, so drink lots of water or other fluids when exercising.
Prepare yourself. During exercise, have a small snack or glucose tablets on hand in case your blood sugar dips too low. Wear a wristband that identifies you as a patient.
As required, make changes to your diabetes treatment strategy. If you take insulin, you may need to reduce your dose before exercising and keep a close check on your blood sugar for many hours after vigorous activity, since insulin may cause blood sugar to spike. delayed hypoglycemia may develop. If you’ve increased your workout habit, you may need to change your therapy.
Medication
When diet and exercise aren’t enough to keep diabetes under control, insulin and other diabetic medicines are used to lower blood sugar levels. However, the success of these drugs is dependent on the dosage amount and time.
What you should do?
Insulin should be stored appropriately. Insulin that has been kept incorrectly or that has passed its expiry date may not be effective.
Inform your doctor about any issues you’re having. If your diabetic drugs cause your blood sugar level to drop too low or rise too high on a regular basis, you may need to modify the dose or schedule.
When it comes to new drugs, be careful. Ask your doctor or pharmacist whether an over-the-counter medicine or a new treatment prescribed by your doctor to treat another illness, such as high blood pressure or high cholesterol, may influence your blood sugar levels.
A different drug may be prescribed in certain cases. Before starting any new over-the-counter medicine, see your doctor to learn how it may affect your blood sugar level.
Illness
When you’re unwell, your body creates stress chemicals that aid in the battle against the sickness, but they may also elevate your blood sugar levels. Diabetes management may be made more difficult by changes in your appetite and daily activities.
What you should do is:
Make preparations ahead of time. Create a sick-day strategy with your healthcare team. Include instructions on how to take your prescriptions, how to monitor your blood sugar and urine ketone levels, how to alter your drug doses, and when to contact your doctor.
Take your diabetic medicine as prescribed. Because of the danger of hypoglycemia, you may need to change your insulin dosage or temporarily decrease or withhold short-acting insulin or diabetic medicine in certain scenarios.
Follow your prevention of diabetes meal plan to the letter. Foods that are easy on the stomach should be kept on hands, such as gelatin, crackers, soups, and applesauce.
To keep hydrated, drink plenty of water or other fluids that don’t contain calories, such as tea. If you’re on insulin, you may need to consume sugar-sweetened drinks like juice or a sports drink to prevent your blood sugar from falling too low.
Alcohol
The liver usually releases stored sugar to counteract falling blood sugar levels. However, if your liver is preoccupied with metabolizing alcohol, your blood sugar level may not get the boost it requires. Low blood sugar may occur quickly after drinking alcohol and can last for up to 24 hours.
What you should do is:
Obtain your doctor’s permission to consume alcohol. What is the best treatment for diabetes issues such as nerve damage and eye disease that might be exacerbated by alcohol? However, if your diabetes is under control and your doctor approves, an alcoholic drink once in a while is OK.
For women of any age and males over 65, moderate alcohol intake is defined as no more than one drink per day, and two drinks per day for men under 65. A 12-ounce beer, 5 ounces of wine, or 1.5 ounces of distilled spirits constitute one drink.
On an empty stomach, avoid consuming alcoholic drinks. To avoid low blood sugar, eat before you drink or drink with a meal if you use insulin or other diabetic drugs.
Carefully choose your beverages. Other alcoholic beverages contain more calories and carbs than light beer and dry wines. If you like mixed drinks, club soda, or seltzer won’t increase your blood sugar.

Make a calorie count. Remember to include the calories from any alcohol you drink in your daily calorie calculation. Incorporate calories and carbs from alcoholic beverages into your diet plan by consulting your doctor or nutritionist.
Check your blood sugar level before going to bed since alcohol may drop blood sugar levels long after you’ve had your last drink. If your blood sugar level isn’t between 110 and 130 mg/dL (5.5 and 7.7 mmol/L), eat something before bed to avoid a drop.
Acquire the Appropriate Amount of Sleep
Americans sleep less than they used to and their sleep is more fragmented. That’s not good news for symptoms of diabetes. Sleep deprivation of 6.5 to 8.5 hours has been demonstrated to raise blood glucose levels.
There is, however, a slight snag. If you receive more than 8.5 hours of sleep per night, you may be at greater risk. As a result, getting the correct amount of sleep is crucial. Try the following suggestions to help you control your sleeping patterns:
- Avoid taking naps, particularly in the afternoon.
- If you can’t fall asleep after around 10 minutes in bed, get out of bed and do something calm that doesn’t include screens—turn off the TV and turn off the phone.
- Every day, not just on weekdays, get up at the same hour. This will train your body to fall asleep at the appropriate moment over time.
- Create a sleep routine. Brush your teeth, wash your face, and perform any other soothing hygiene procedures in the same order and manner. This aids in the preparation of your thoughts for bedtime.
Conclusion
The more you understand the elements that affect your blood sugar level, the better you’ll be able to predict variations and prepare appropriately. Ask your diabetic healthcare team for assistance if you’re having problems maintaining your blood sugar level within your goal range.
So, at the end of the article, we would recommend you take action if you are seeing any diabetes symptoms and see a doctor. Follow our diabetes tips and diet, exercise properly, and choose your meal wisely.
























No Comments